Hi, I’m Kevin. I’m 49 years old, I’ve been married for 23 years. I have two boys in college. I’m 6-foot tall and weigh almost 190 pounds. I have worked for Men’s Health for the past 8 years and I generally live an active, healthy lifestyle.
And five weeks ago a doctor unclogged an artery in my heart that might have left me dead or disabled before Christmas.
“I’d say I dodged a bullet,” I told a friend, “but that implies that I saw it coming.” It’s more like I was standing one foot in the street when a city bus narrowly missed me.
SEVEN WEEKS ago, I felt something in my chest. It was not quite pain, not quite pressure. Mostly an awareness, usually on the extreme left side of my chest. Sometimes it would jump to the extreme right side.
Initially I thought I had tweaked a muscle while serving as part of a test panel for an upcoming fitness DVD (Oh, the perks of being a Men’s Health editor).
Six weeks ago, the something hadn’t gone away, and I had to admit that it wasn’t a muscle tweak. The discomfort was coming from within my chest—like those floor-drops-out-below-you moments in a horror movie where the police let you know that the maniac’s call was placed from INSIDE your house!!!
The realization came upon me like a dark cloud (cliched, but exactly how I felt). My family has a long history of heart disease. My dad had quintle-bypass surgery in 1985, at the age of 44. Even worse, when he awoke from the procedure, his surgeon asked him when he had his heart attack. My dad stared at him dumbfounded. He had never had a heart attack, he insisted. The surgeon said the scar tissue around his heart argued otherwise. That set off a family parlor game: When Did Dad Have His Heart Attack? We finally landed on a most likely candidate: Family vacation, a few years earlier. The San Diego Zoo. He thought he was coming down with the flu and headed back to the hotel, where he slept it off. He was back in the driver’s seat, driving us to LA, the next day. Call it drive-thru rehab. That was my dad. He passed away five years ago, at 70.
His dad died at the age of 42, in 1944. An Irish immigrant driving a bakery truck, he flipped it over on the streets of New York. They pulled his dead body from the truck. Nobody did autopsies on poor Irish truck drivers back then, so the cause of his death remains a medical mystery.
It’s pretty much like that on my dad’s side of the family. His cousin, in Dublin, has suffered from painful angina for years, and has enough stents to open a cardiac medical supply store.
And still, I figured that if I did enough good things—stayed active, ate pretty well, managed stress and my weight—that I could stay ahead of this shadow. But here it was.
I called my GP, let’s call him Doctor V, and asked to move up a scheduled checkup by a week.
Things were going fine at my checkup. My blood pressure was a little high but that was understandable because I was nervous. I bent over a table, grimaced, and found out second-hand (pun intended) that my prostate was a small, supple thing of beauty. Dr. V and I talked about my chest discomfort and he thought it sounded muscular. Lauren the Nurse would come and give me an EKG and I could go home.
Except that, after taking the EKG and disappearing for a second, Lauren came back and asked me to stick around. Dr. V. wanted to talk with me.
The shadow closed in.

Here’s a quick primer from EKG 101: In a healthy EKG, there are a series of waves, labeled P through U. P marks the contraction of the atria, and is a slight turn upward; QRS is a small down-big up-small down movement that marks the contraction of the ventricle; and the T is a small upward movement that marks the re-set (repolarization) of the heart before it pumps again. The P, R, and S are all supposed to go up. In mine, several of the leads showed the first two waves going up, then the third sagging downward. That’s an inverted T wave, and the T stands for Trouble. It can be a sign of blockage.
But maybe not. My doc wasn’t sure what to do. We didn’t have a history together. In fact, this was our first time as doctor and patient (we knew each other from his treating my 18-year-old son). EKGs are not exact science, he explained. In fact, I could have had this abnormality in my heart beat since I was born. “My gut tells me this isn’t something we should ignore,” he said. “Would you mind going to the ER?”
I didn’t, and I did. The docs drew blood to check for specific inflammation markers and to run a blood panel, and did another EKG. The decision: I wasn’t having a heart attack but I needed more tests, specifically a nuclear stress test.
SIX DAYS LATER, I woke up the morning of the stress test feeling better than I had in two weeks. No pain at all. A ghostly absence of sensation.
The stress test involved injecting a radioactive dye in my bloodstream, then imaging my heart before and after a period of activity. It was pretty cool—I’d been experiencing this long enough that my curiosity was now routinely trumping my fear—and strangely liberating. The ER doc had made a point of telling me not to go too hard until that test, especially after I told her I had pushed a sled with 425 pounds on it around the gym trying to trigger a reaction that would confirm this was angina (it didn’t work). So the chance to exert myself on a treadmill felt good. I was able to walk fast, then run, for about 9 minutes. I got my heart to 160 beats per minute. No pain. Maybe this is going to be OK, I thought. I laid down for the after-exercise set of images and went home.
My brand-new cardiologist, Dr. Matthew Levy, called me on my cell that evening. I was shooting baskets on my driveway.
“It doesn’t look good,” he said. “You definitely have a blockage. I need you to come in two days from now to get cathed. We’ll take a look at it, and if the blockage is severe enough, we’ll perform an angioplasty.”
We talked for a few more minutes, then he said. “I don’t know you very well, but you don’t sound surprised.”
I was, and I wasn’t.
TWO MORNINGS later, I was on an operating room table in Paoli, Pa., the object of a cardiac catheterization. I was drugged but not knocked out; it was more dreamy than blotto. While I know that I was half-there, I have no useful memories from the operation or from the couple hours afterward.
 I would later find out that my left anterior descending artery (known in heart circles as “the widowmaker”), which snakes down the front of my heart, was about 95% blocked. A stent was put in place to open the blockage. I was out of the hospital within 24 hours of the procedure, with little to show for it other than a broken night’s sleep and a minuscule incision in my right wrist, where the catheter was inserted. The site was a little swollen and bruised. I sat outside on the deck of a local winery at 4 p.m. that day, sipping a half-glass of red wine, enjoying the afternoon sun, listening to a jazz band, and insisting to friends that I had indeed been a patient in a hospital that morning.
I would later find out that my left anterior descending artery (known in heart circles as “the widowmaker”), which snakes down the front of my heart, was about 95% blocked. A stent was put in place to open the blockage. I was out of the hospital within 24 hours of the procedure, with little to show for it other than a broken night’s sleep and a minuscule incision in my right wrist, where the catheter was inserted. The site was a little swollen and bruised. I sat outside on the deck of a local winery at 4 p.m. that day, sipping a half-glass of red wine, enjoying the afternoon sun, listening to a jazz band, and insisting to friends that I had indeed been a patient in a hospital that morning.
I have a new regimen of three pills—baby aspirin, the blood thinner Effient, and the statin Lipitor—that I take daily. I’ve run a few times and the biggest issue has been my balky left knee. I am about a minute-a-mile faster than I’ve been for the past two years. I wonder if having an almost catastrophic blockage of the biggest artery feeding my heart is actually an advantage. Am I now turbo-charged? Am I asking for some karmic fuck-job for even thinking this way??
My cardiologist tells me I was days, or weeks, or maybe a month or two from a possibly devastating heart attack.
I feel pretty damn lucky.
THE QUESTION, of course, is this: Shouldn’t I have seen this coming?
Medically, the answer is surprisingly equivocal.
How to treat folks like me remains controversial, said Dr. Spencer Nadolsky, the medical editor of Examine.com who has a practice in Olney, Md.
“It really depends,” he said, “because someone with a low risk—a slightly elevated cholesterol level but not a family history, they’re clean, their blood pressure and blood sugar is all fine—they can have slightly higher lipid levels without as much of a risk as someone with those risk factors. You may have to treat 100 people like that to avoid one heart attack over five years.
“Now someone with higher risk, you may be treating 50 or less people to prevent one heart attack in five years. It is one of those things we argue all the time. It’s primary prevention vs. secondary prevention.
“What you’re doing now is secondary prevention. You’ve already had a coronary issue and now you’re trying to prevent the second event, a heart attack. And other people who have initially high cholesterol [but no cardiac disease] may be on statins too. What we find is that statins may be more helpful in secondary prevention than in primary prevention.”
So there’s a medical argument that makes me look less like an idiot. Yes, I had a family history, but my blood panels over the years were borderline. Cholesterol right around the 200 mark, with not a lot of the good stuff (HdL). Triglycerides on the high side, but not crazy. Over the years, a doctor would look at the panel, then look up at me, then decide it all bore watchful waiting.
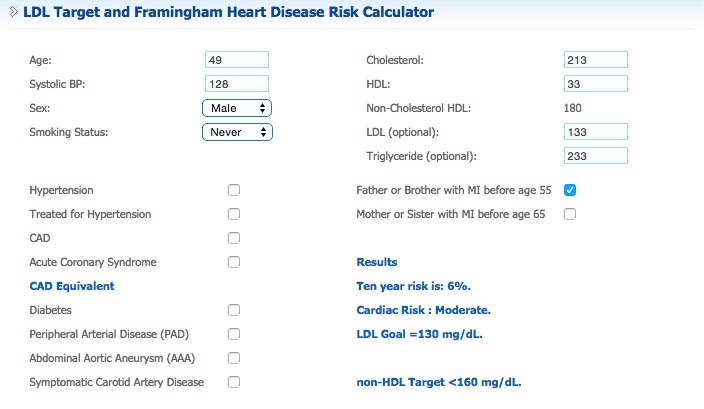
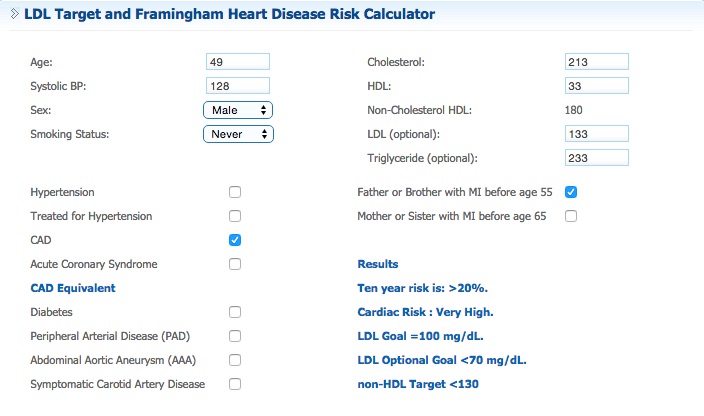
Here is a recent blood panel and a popular risk calculator. If I don’t know I have cardiac artery disease, my 10-year risk of heart attack is 6%. It jumps to more than 20% if I do know. Note that I copped to a family history in both examples.
So we watched—until I screwed up. And here’s where we move beyond medical cover into my own accountability. Because I stopped seeing my old GP after we disagreed over how much activity a guy in his 40s should engage in (I said more, he thought it was asking for injuries). He moved out of the area soon after—and for 6 years or so, nobody watched anything.
It’s the most obvious advice one could receive: Find a new GP. But I didn’t. I can say I was busy, that I was occupied by family and career and anything that could keep me from going to the doctor. That I felt fine.
But the truth is as long as I was feeling good I didn’t want anyone spoiling my party. So I didn’t look while I stepped in and out of that city street.
Anyone else? Show of hands, please. Thought so. We’re a big club, with a lot of turnover. in 2012, more than one-quarter of all guys avoided a checkup with a doctor.
Late this summer, with my 50th birthday just months away, I decided to find a doctor. I made an appointment with a general practitioner who impressed me with his care of my son, who has several health issues. I set up the appointment before I ever felt a twinge in my chest. In my blacker moments, after my chest tingled and before I got to the doctor’s office, I thought, Nice job, Kevin. You invoked this motherfucker.
Except I know I didn’t. And that my decision to move up my checkup may have saved my life.
So here I am, and here’s what I’m doing.
I’M CLEANING UP MY DIET. I love salty snacks and good ol’ Coca-Cola. Both are getting dialed WAY DOWN. The great thing about cravings is the longer you go without them, the easier it is in the moment. My Coke intake is down to about one a week. Pretzels, once a month.
Dr. P.K. Shah, of Cedars-Sinai Hospital in Los Angeles and a member of the Men’s Health advisory board, encouraged me to lean toward a Mediterranean Diet. My cardiologist, Dr. Levy, made it even simpler: eat fish twice a week. Dr. Nadolsky said to snack on nuts and find a way to consume 4 teaspoons of extra virgin olive oil every day.
Since this episode began, I’ve dropped 6 pounds, to 182. I’d like to settle in for now close to 180 pounds.
I’M MOVING. Research says that 30 minutes of moderate exercise 4-5 times a week is where I should start, and I am. But there’s some that suggests that more intensive exercise provides additional benefit. My doctors have told me I’m under no restrictions within reason. My aim is to push myself hard to keep my pipes as clean as possible. I am pushing the sled again, and running suicides at a local basketball court. Suicides suck—but not doing them sucks worse, I think.
I’M RECONNECTING WITH THE DOCTOR. I’ve learned my lesson. I will continue to check in with my GP (Dr. Graham Vigliotta) and cardiologist (Dr. Matthew Levy, Cardiology Consultants of Philadelphia).
The thing is, your 40s are a time of transition and not all of it is positive. Risks accumulate over time, and I cannot ignore them. I am taking statins—with coronary disease now determined, that’s a no-brainer, says Dr. Nadolsky.
If any of this story resonates with you, start at the beginning. If you don’t have a GP, get one. If you haven’t seen yours in a while, see her or him. If you have a family history of heart disease, get a baseline EKG by 40, younger if you have other risks factors (obesity, hypertension, generally shitty habits).
At the same time, and I hope this doesn’t sound like I’m backing out here, I refuse to be defined by my illness. I am not a diagnosis. Going forward, my goal is to be aware of it AND work with it to thrive.
I’m hanging my hat on what Dr. Shah told me: “Although having heart disease at a young age indicates a serious predisposition, proper lifestyle and medical management can largely control that risk and is compatible with a normal life span.”
“People with conditions like yours live into their hundreds,” said my new best friend, Dr. Nadolsky.
I’M STAYING POSITIVE. People who have coronary disease who have a positive attitude tend to stick with behaviors that provide better outcomes, like exercise and compliance in taking meds, reports a study in Psychosomatic Medicine.
Beyond that seemingly self-evident bit of news, I have a fresh new frame: I’m on a journey from happily ignorant to scared shitless to soberly, joyously aware. I know that I was extraordinarily lucky. A very-real and long-unacknowledged peril never turned into a calamity. I know people right now who weren’t cut such a break.
One thing I’ve done is apologize to my wife for letting this all skulk in the shadows long enough that she needed to wait an hour for me to return from a hospital cardiac cath operating theater. Just before I headed in, she looked down with her eyes brimming, and said, “You know you mean the world to me.”
I know, and I know that I am part of a lot of people’s worlds. I will be a better steward of her care, and their care, going forward.
I’M TREATING MY LIFE AS A GIFT. I’m sharing this with the intention that it helps me (and you) live in awareness of the shadows and the light of our experience.

Leave a comment